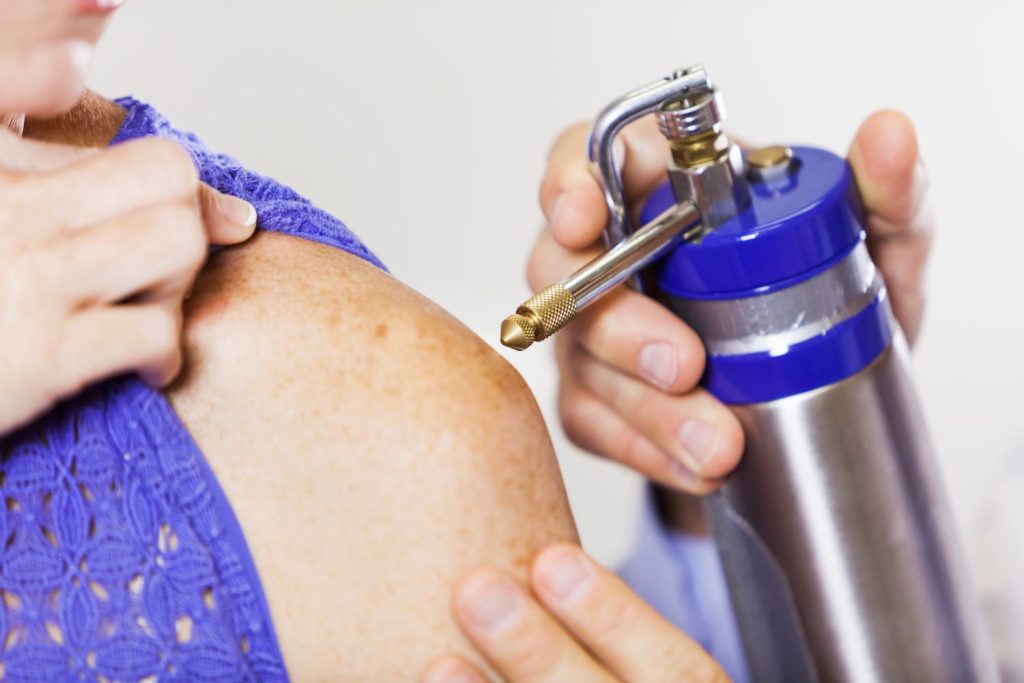
Cryotherapy is a treatment where extreme cold is used to destroy abnormal skin cells. Instead of burning with heat, the cold causes controlled cell damage.
It is commonly used for:
Please contact the clinic if you notice increasing pain, redness, or swelling after 3 days, as this may indicate infection.
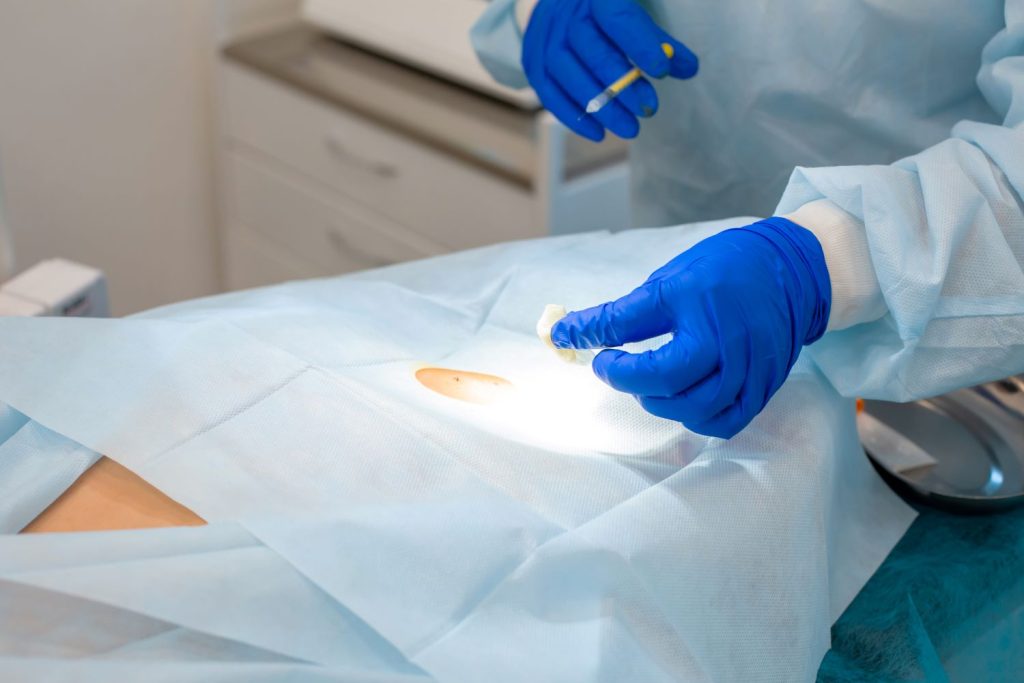
Curettage and cautery is a technique where skin cancers are removed by scraping and heat treatment. It can be a good option for certain types of skin cancer, particularly superficial lesions, and allows multiple spots to be treated in a short session.
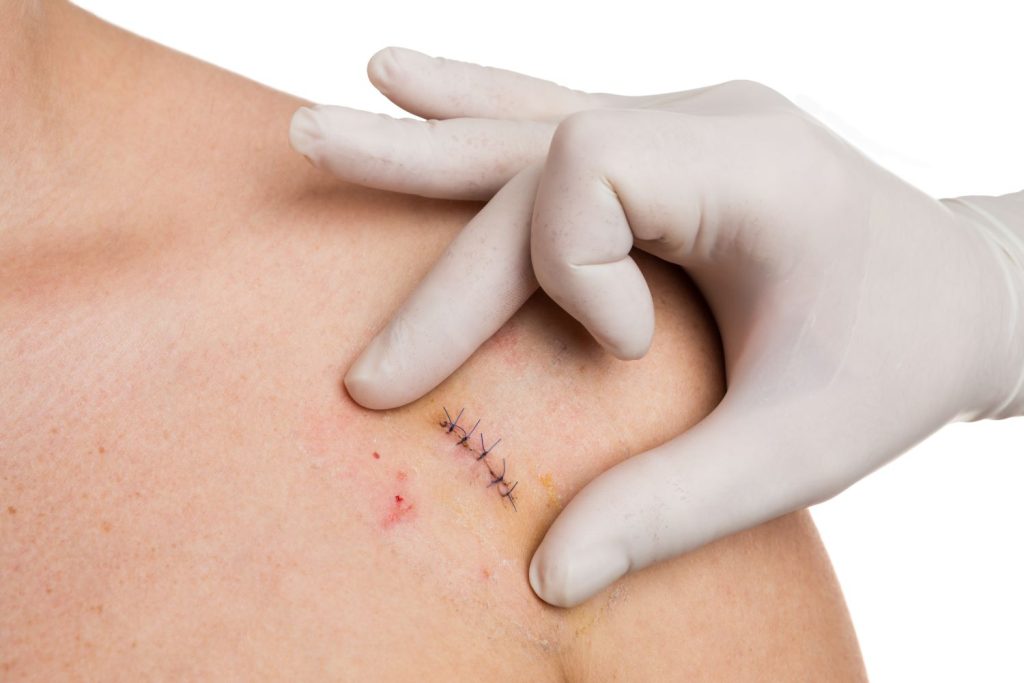
After healing, the treated skin may look different:
The vast majority of skin cancers can be removed under local anaesthetic with a simple elliptical excision.
Sometimes a wound cannot be closed directly because there isn’t enough loose skin. In these cases, a full-thickness skin graft may be used.
A skin flap uses tissue adjacent to the wound to close the defect.
In select areas, it may be better to leave the wound open and allow it to heal naturally. This is called secondary intention healing.
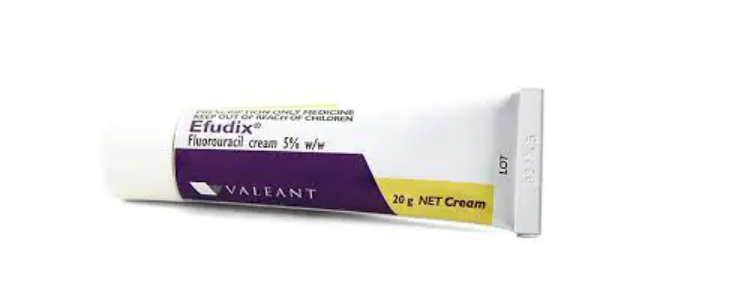
Solar keratoses (actinic keratoses) are precancerous sun-damaged lesions that appear as rough, red, scaly patches on areas like the face, ears, scalp, forearms, and hands. While most are harmless, a small number progress to squamous cell carcinoma each year (1 in 100 to 1 in 200 risk per spot per year).
Efudix is a “field treatment,” meaning it targets both visible lesions and subclinical precancerous cells in the surrounding skin. This makes it particularly effective when multiple lesions are clustered in one region.
Bowen’s disease (SCC in situ) is an early form of squamous cell carcinoma where cancerous cells are confined to the top layer of skin. Lesions usually appear as red, scaly plaques that slowly enlarge.
Efudix can be a very effective non-surgical treatment for Bowen’s disease, especially on areas where surgery might be difficult or leave large scars.
A review is essential after treatment to ensure the lesion has resolved. If there is incomplete clearance, surgery or another therapy may be recommended.
⚠️ Contact the clinic if you have any concerns. Whilst discomfort and some redness is common, we do not expect pain that interferes with sleep, your usual activities or requires paracetamol.
Basal cell carcinoma (BCC) is the most common and least dangerous form of skin cancer. A common subtype is superficial BCC, which often looks like a shiny pink or red patch or a dry scaly area that slowly enlarges over months or years.
Aldara works by stimulating your immune system to recognise and destroy cancer cells. The active ingredient, imiquimod, activates immune cells that then attack the abnormal skin. This process causes redness, flaking, scabbing, and sometimes soreness in the treated area — all signs that the cream is working. Very rarely, people can experience flu-like symptoms.
Sachets: single-use only. Discard after opening.
Pump dispenser: replace cap after use. Store below 25 °C. Use within 4 weeks of opening. Do not freeze.

